WorkCompWire
Full article on: workcompwire.com
Frank Raneri, Senior Vice President, Paradigm Specialty Networks
To deliver value, effective specialty networks must focus squarely on novel solutions for emerging cost drivers.
Managed care firms and entrepreneurial businesses have a strong history of identifying key trends in claim cost exposure and building solutions to address growing areas of concern. Dramatically shifting from indemnity to medical expense, responding to the opioid crisis, and navigating the COVID-19 pandemic, are just a few examples of how our sector’s leaders have repeatedly found ways to contain costs. Innovative specialty network solutions have regularly been essential to addressing these issues and responding to underlying drivers of spend.
In today’s environment, workers’ comp payers are increasingly encountering distinct but interrelated forces that are putting pressure on medical costs. The Bureau of Labor Statistics consistently reports that hospital services lead all consumer segments in cost inflation—and workers’ comp is feeling the impact. Specialty segments of outpatient surgical spend, such as joint replacements, are compounding the trend through increased frequency and outsized costs. To continue delivering value, networks must be ready to respond to these inflationary trends with forward-looking solutions.
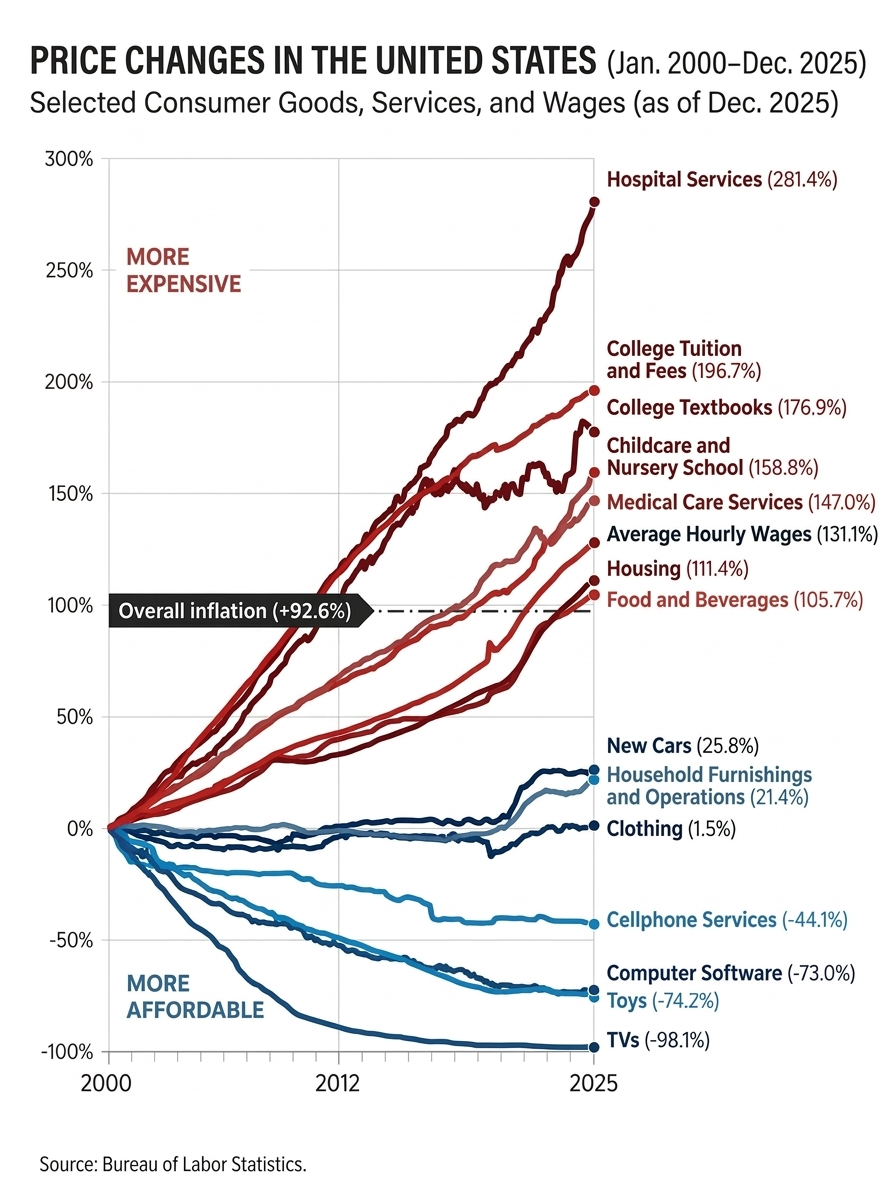
What’s driving up medical costs in workers’ comp?
From ever-rising facility fees to the impact of tariffs on surgical implants, here are a few of the key cost drivers that networks must analyze and address:
- Rising facility costs: With up to 40 cents of every workers’ comp medical dollar spent on facility-related expenses, high hospital fees directly shape the cost of work-related claims. One particularly alarming trend shows some hospitals charging workers’ comp payers significantly higher rates for outpatient surgeries when compared to other insurers. The Workers’ Compensation Research Institute (WCRI) estimates this can result in an additional $7,500 to $22,000 per procedure.
- Growing provider consolidation: Consolidation has accelerated in recent years, with more than 470 hospital mergers between 2016 and 2024. Limited competition enables large health systems to exert significant influence over pricing, with aggressive network negotiations often resulting in only modest discounts.
- Inconsistent fee schedules: WCRI estimates that states without cost controls or fee schedules see payments 61% to 134% higher than those in regulated states, and 69% to 217% higher when payments are limited to a percentage of hospital charges. And unlike group health insurance, where patients may opt for lower-cost facilities to limit out-of-pocket expenses, injured workers typically incur no direct costs and have limited influence over surgical site selection.
- Cost drivers in surgical implants: From 2021 to 2024, costs for surgical implantable devices in the U.S. rose sharply. During this time, the S. Producer Price Index for surgical and medical appliances reached record highs—about 8% to 9% above pre-pandemic levels. Tariffs imposed in 2025, ranging from 10% to over 50%, further escalated implantable device costs. Surveys indicate that 82% of hospital executives expect a 15% increase in overall hospital costs due to tariffs.
What does innovation look like for specialty networks?
As an industry, we see it in the headlines and in our data: routine, non-emergent surgical procedures in the hospital setting now pose a significant economic headwind.
Think of the innovation arc in workers’ comp networks as analogous to developments in automotive safety, which have dramatically reduced the severity of automobile-related claims over the past several decades.
Like a car’s seatbelts, broad-based networks represent a core “safety feature.” You won’t find a credible managed care program that operates without a strong, broad-based network. The emergence of specialty networks, meanwhile, can be compared to airbags. Once seen as a novel supplement to base networks, specialty networks now often operate in the primary position—adding targeted security across network configurations.
But automobile safety has continued to evolve well beyond seatbelts and airbags. Today’s vehicles are equipped with cameras, lane assistance, pre-crash detection, and driver attention alerts. Given the dramatic rise in facility costs in recent years, specialty networks should be just as robustly equipped.
Paradigm’s Surgical Cost Management Plus program modernizes network configuration to address these growing cost management pressures. By combining the core elements of our orthopedic specialty network, a best in-class implant review product, and innovative payment integrity tools, we deliver an all-in-one solution for reducing hospital outpatient surgical expenses. With inflationary trends showing no signs of slowing, Paradigm remains committed to setting new standards in savings through network strength and innovation.